The patient was referred by a general practitioner. She couldn't perform any overhead activities, due to increasing pain when lifting the arm sideways (abduction). Furthermore, she had lot's of problems with falling asleep. She reported a VAS 7. The pain and functional problems started 2 months ago. The moment of onset was not totally clear.
I scanned the whole shoulder protocol. Of all images made in the whole protocol I will share the following clinical relevant images:
1) Supraspinatus tendon statically: the patient was in modified Crass position. The transducer placed in transverse or longitudinal over the supraspinatus tendon on the ventral shoulder.
2) Supraspinatus tendon dynamically: the patient had the arm hanging by her side. The transducer was placed in transverse over the coracoacromial ligament, longitudinal supraspinatus and close to the acromion.
3) Long head of the biceps tendon: the transducer was placed on the ventral shoulder, covering the intertubercular groove, and in transverse over the biceps tendon.
4) Subscapularis tendon: the patients arm was placed in external rotation. The transducer was placed longitudinally over the subscapularis tendon. To double check the pathology findings several left/right comparisons were made. Images were analyzed by using the SonoSkills pathology checklist.
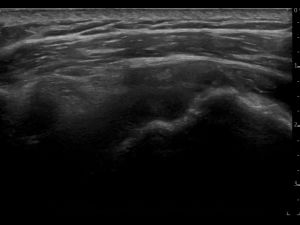
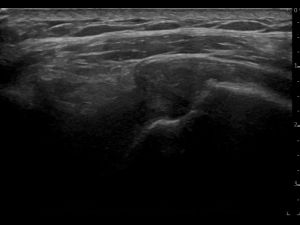
- SHAPE: The supraspinatus tendon does not show it's normal shape anymore. Some parts appear to be thicker than normal (especially the anterior supraspinatus tendon near the rotator interval), other parts appear to be subtly thinner than normal. The bone of the anatomical neck and greater tubercle seems to be irregular. The SASD bursa has increased in thickness and cross-sectional area: not only near the supraspinatus, but especially also near the long head of the biceps tendon and subscapularis tendon.
- ECHOGENICITY: the supraspinatus tendon shows mixed zones of echogenicity: hyperechoic, hypoechoic and anechoic. Observing the thickened hypoechoic parts one can conclude the tendon is definitely tendinopathic. More worrisome are the anechoic parts spreaded around the tendon: articular sided, mid tendon and also bursal sided. The anechoic parts vary in size, and some seem connected. Small hyperechoic particles can be seen near the greater tubercle, most likely some calcification deposit. The SASD bursa swelling is anechoic, indicating normal bursal fluid.
- CONTINUITY: Because some anechoic parts seem to be connected, we can regard this supraspinatus as having a full thickness tear. The biggest anechoic zones, torn fibres, can be seen around the anatomical neck and near the bursa. Since there's no retraction, and other parts seem to be connected, it's also a partial width tear.
- DOPPLER: There is a very small positive Doppler signal presence in the SASD bursa. The tendon itself shows no signs of neovascularization.
- FUNCTIONAL: A clear impingement can be seen between supraspinatus / SASD bursa and the coracoacromial ligament during active abduction.
Based on the ultrasound findings and SonoSkills pathology checklist analysis I concluded: - Full thickness/ partial width tear supraspinatus tendon - Potentially other partial tears: articular sided near anatomical neck, and mid tendon. - Tendinopathy supraspinatus tendon - Mild sign of neovascularization - SASD bursa effusion - Primary impingement of the supraspinatus tendon and SASD bursa with the coracoacromial ligament during active abduction.